Vitreo-Retina
- Services
- Vitreo-Retina
Facility – Vitreo-Retina
- Indirect Ophthalmoscopes
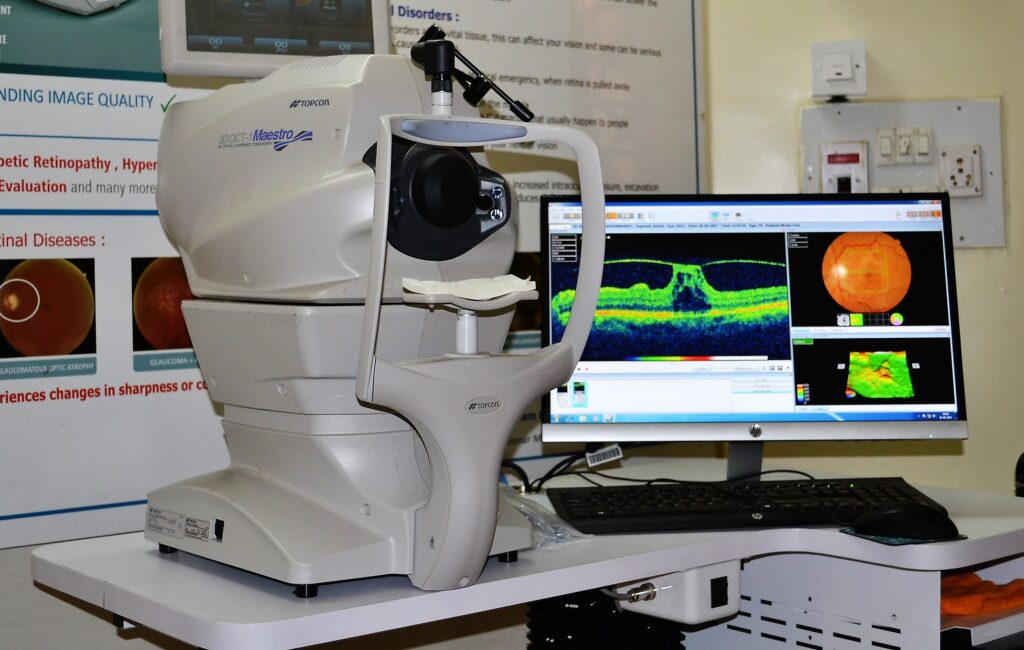
- Digital Retinal Scan
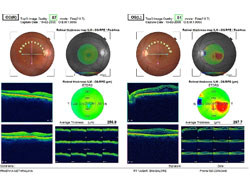
- OCT
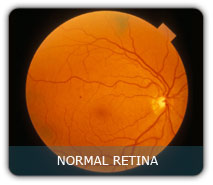
What is a Retina?
Retina is the light sensitive layer at the back of the eye. Which is like a film of the camera on which light falls and a person is able to see. Diabetes affects the blood vessel of the retina.
Prolonged high blood sugar in a diabetic patient produces changes in the blood vessels all over the body. The damage to the blood vessels of the retina is called Diabetic Retinopathy. The only blood vessels in the body that can be seen in the natural state are the retina blood vessels.
How can diabetes affect the eye?
- It may lead to frequent fluctuations in vision.
- Cataract in young age,
- Temporary paralysis of the muscles controlling the movement of eyes, leading to double vision.
- The most significant complication of diabetes in the eye is diabetic retinopathy and its complications.
There are various stages of diabetic retinopathy
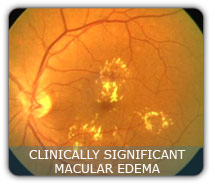
NON-PROLIFERATIVE or background diabetic retinopathy:
When blood vessels in the retina are damaged, they can leak fluid or bleed. This causes the retina to swell and the contents of the blood to deposit which are called exudates. This is an early form of diabetic retinopathy and may not lead to any decrease in vision, since the center part or the most light sensitive part is not affected but it can lead to other more serious forms of retinopathy that affect the vision if left untreated.
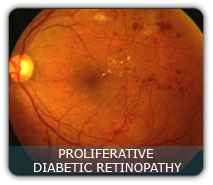
PROLIFERATIVE diabetic retinopathy:
This is an advanced stage of diabetic retinopathy, where the blood supply to the retina is compromised as response to this, new fragile blood vessels grow on the surface of the retina (revascularization). These new vessels are very fragile and bleed easily. These may lead to serious vision problems if they bleed into the vitreous (the clear, jelly-like substance that fills the center of the eye) which is known as vitreous hemorrhage. This prevents the light from reaching the retina and thus can blur the vision. The new blood vessels and the bleed into the vitreous can also cause scar tissue to develop, which can pull the retina away from the back of the eye. This is known as tractional retinal detachment, and can lead to blindness if untreated, this advance diabetic retinopathy usually require surgical intervention and are also not very successful.
In addition, abnormal blood vessels can grow on the iris (the colored part in the front of your eye, which can lead to glaucoma).
What are the risk factors for diabetic retinopathy?
- Uncontrolled and fluctuant Diabetes
- The longer the person has diabetes, the greater are his/her chances to develop diabetic retinopathy. Almost 80% of people, who have diabetes for more than 15 years or more, have some damage to the blood vessels in their retina.
- The other risk factors are high blood pressure, anemia, kidney diseases, and pregnancy.
Can something be done to prevent diabetic retinopathy?
How can one know if he/she has diabetic retinopathy?
How frequently should one get one’s eye examined?
How is diabetic retinopathy treated?
In the initial stages no treatment may be requires only good control of diabetes ,but as the condition progress one may require laser treatment and in advance stages like in proliferative diabetic retinopathy surgery may also be required to maintain the vision.
Patients with diabetes develop CATARACT earlier than normal people; they may be associated with PRIMARY OPEN ANGLE GLAUCOMA and can also develop nerve palsy.
Highlights of Diabetic Retinopathy
- Diabetic retinopathy can be assessed only by retinal examination by an OPHTHALMOLOGIST only.
- Retinal test is not same as glasses testing.
- Computerized eye testing in an optical shop does not check your retina
- Beware! Early stages of diabetic retinopathy will not produce any sight loss.
- Good control of your sugar levels and at least an yearly check by your OPTHALMOLOGIST is a necessary.
Videos
Make An Appointment
Opening Hours
- 10.00 AM - 08.00 PM
- 09.30 AM - 05.00 PM
- Holiday
For Online Consultation
Make Appointment
- 10.00 AM - 08:00 PM , Monday - Friday
- 9.30 AM - 05:00 PM , Saturday
- Holiday , Sunday
- https://bit.ly/3rkHIwO