Cornea
- Services
- Cornea
Facility – Cornea
- What is a Cornea?
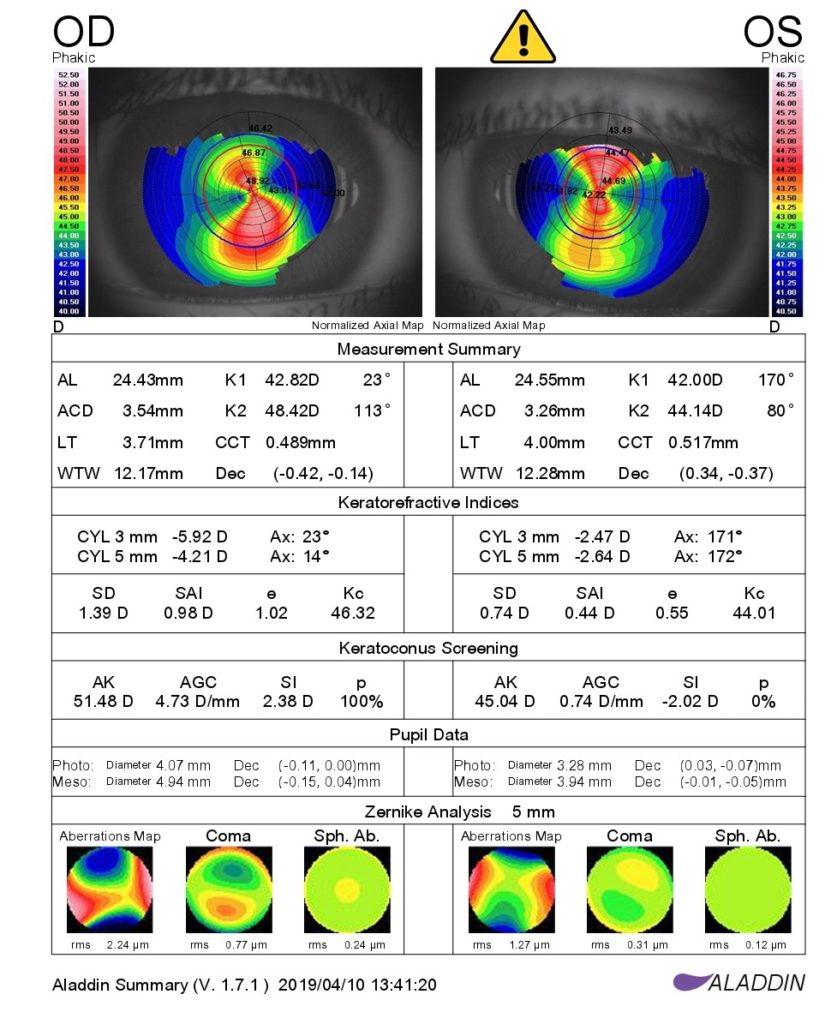
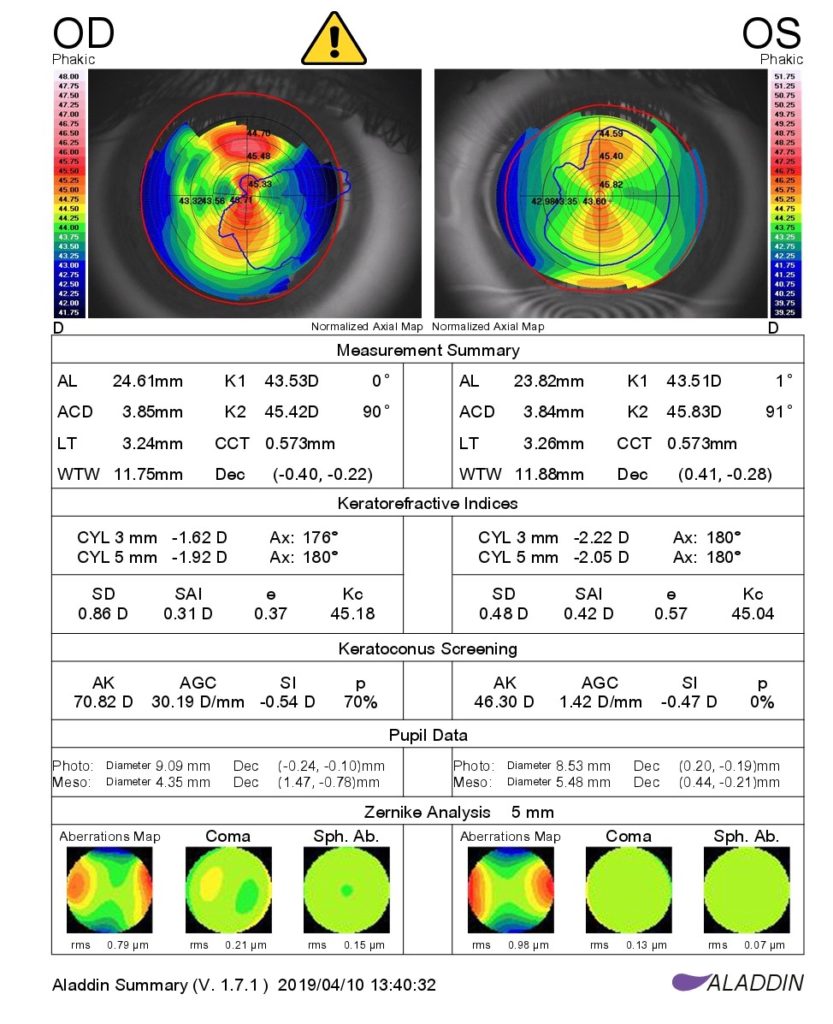
- WHAT IS KERATOCONUS?
The cornea is the transparent portion of the eye which allows light to enter and performs two-thirds of the focusing tasks.
The cornea does indeed allow light to enter the eyeball and the cornea’s convex shape focuses that light towards the pupil and another structure called the lens.
Often appearing in the teens or early twenties, keratoconus is a progressive disease in which the normally round cornea thins and begins to bulge into a cone-like shape. This cone shape deflects light as it enters the eye on its way to the light-sensitive retina, causing distorted vision. Keratoconus can occur in one or both eyes.
The foldable lens is injected through the small opening and it opens inside the eye to the normal size. Advantages- Wound healing is faster
- Wound stability is better
- since the entire surgery is done through a very small opening
- Induced astigmatism is minimal
- Decreased glare
WHAT ARE THE SIGNS AND SYMPTOMS OF KERATOCONUS?
- Astigmatism
- Blurred Vision – Even while wearing Spectacle & Contact Lens
- Glare at Night
- Light Sensitivity
- Frequent Prescription Change in Spectacle & Contact Lens
- Near Sightedness
- Rubbing of the Eye
- Ghost Images
KERATOCONUS
New research has demonstrated a relationship between malfunction of beneficial enzymes found within the eye’s surface and an accompanying chemical imbalance that leads to toxic damage and thinning of eye tissue. Because keratoconus can be found in extended families, this improper functioning of beneficial enzymes appears to have genetic causes about 5% of the time. Eye damage from keratoconus also can be linked to factors such as overexposure to sunlight, improper fittings of contact lenses, excessive rubbing of the eye, and continual (chronic) eye irritation.
- Keratoconus is usually detected when the patients reach their 20’s. For some, it may advance over several years. For others the progression might reach a certain point and stop.
- Keratoconus is not visible to the naked eye except during the later stage of the disease. In severe cases the cone shape is visible to an observer when the patient looks down and the upper lid is lifted. When looking down, the lower lid is no longer shaped like an arc, but bows outward around the pointed cornea. This is called Munson’s sign.
- Special corneal test called ‘Topography’ provides the doctor with detail about the cornea’s shape and is used to detect the progression of the disease. A ‘Pachymeter’ may also be used to check the thickness of the cornea.
The first line of treatment for patients with keratoconus is to fit rigid gas permeable (RGP) contact lenses. Because this type of contact lens is not flexible, it creates a smooth, evenly shaped surface to see through. However, because of the cornea’s irregular shape, these lenses can be very challenging to fit. This process often requires a great deal of time and patience. When vision deteriorates to the point that contact lenses no longer provide satisfactory vision, corneal transplant may be necessary to replace the diseased cornea with a healthy one.
ABOUT C3R
At Pradnya Nethralaya patients can avail of the facility of C3R.
It is done in the Operation Theatre. The Cornea is sensitised with Riboflavin and the exposed to UV light for 30 mins.
This results in a chemical reaction that create covalent bonds which strengthen the corneal stroma.
REMEMBER
VIDEOS
Make An Appointment
By Filling the form
Opening Hours
- 10.00 AM - 08.00 PM
- 09.30 AM - 05.00 PM
- Holiday
For Online Consultation
Make Appointment
- 10.00 AM - 08:00 PM , Monday - Friday
- 9.30 AM - 05:00 PM , Saturday
- Holiday , Sunday
- https://bit.ly/3rkHIwO